Nudging people out of the coverage gap, cont.
In my last post, I noted that on May 5 CMS finalized a rule that patches a bit of the coverage gap afflicting low-income people in 13 remaining states that have refused to implement the ACA Medicaid expansion.
In those states, eligibility for ACA premium subsidies begins at incomes above 100% of the Federal Poverty Level (FPL). State residents with incomes below that threshold who do not qualify for Medicaid under the states' restrictive criteria get no government help to pay for coverage. Some 2 million adults are in this gap.
In its annual Notice of Benefit and Payment Parameters for the ACA marketplace (NBPP 2021), published May 5, CMS announced that if an applicant estimates an annual income above 100% FPL, but the "trusted data sources" tapped by HHS indicate an income below that threshold, the applicant will no longer be required to provide documentation of the projected income.* The rule change is in prompt compliance with a court decision delivered on March 4 in response to a suit filed by Columbus, Ohio and several other cities (and two individuals) seeking to overturn several Trump-era rules for the marketplace -- including a requirement that exchanges demand documentation in this situation.
In effect, anyone in a nonexpansion state otherwise eligible for marketplace coverage can now claim an income in excess of 100% FPL and become subsidy eligible. Thanks to the subsidy boosts implemented in the American Rescue Plan in March, generous coverage with low out-of-pocket costs is available to enrollees with income below 150% FPL. An emergency Special Enrollment Period running through August makes that coverage available now (on the first of the month following enrollment).
ACA marketplace applicants provide the required financial data under penalty of perjury. And the federal government is not in the business of encouraging people to defraud it. Indeed, the decision requiring this rule change (by Federal District Court Judge Deborah K. Chasanow in City of Columbus, et al. v. Cochran) is predicated on the lack of evidence that enrollees fraudulently inflated their income to qualify for subsidies before the Trump administration mandated documentation in this situation in advance of Open Enrollment for 2019.
Judge Casanow, however, also cites comments submitted in response to the Trump administration proposed rule in 2018 noting that "'low-income consumers are more likely to experience variance in their income levels'...many 'work in part-time or in hourly positions,' 'rely on multiple part-time or part-year jobs,' or 'work in cash industries, such as food service, where tip-income makes up the largest portion of their earnings'" (p. 22).
These conditions not only make it difficult to document income -- the Judge's chief concern -- they make it difficult to project annual income, as a marketplace applicant must do, either for the year following (during Open Enrolment in late fall/winter) or for the year in progress (when the applicant obtains a Special Enrollment Period).
CMS could nudge people toward projections that will get them over the 100% FPL threshold -- simply by marking that threshold out, both in the application and in the "see plans and prices" preview tool on HealthCare.gov. In that tool, a user provides an estimate of income along with information about household members and their ages; subsidized plan prices are estimated on that basis.
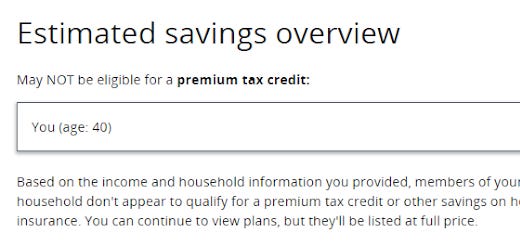
At present, a user who enters an income below 100% FPL in a nonexpansion state will get results showing no eligibility for subsidy, with no explanation. Here are the results for a single adult in Texas entering an income of $12,000, or 94% FPL:

No soup for you. Why? Is my $1000/month income too high? No clue provided.
Here is the result when the income entered is $13,000 (102% FPL):
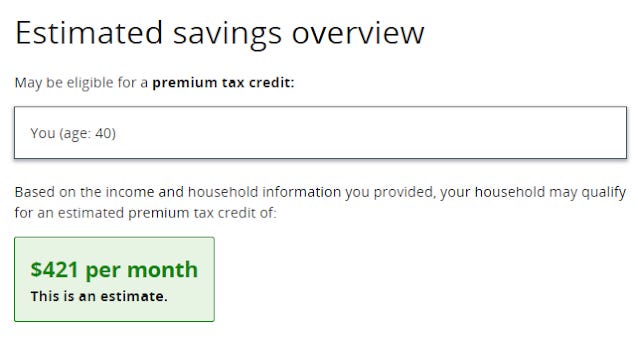
Sounds better, no? If I click through to plans available (after a couple of misleading screens that are a subject for another day), the first plan I see looks like a pretty good deal (as in: zero premium, zero deductible**):
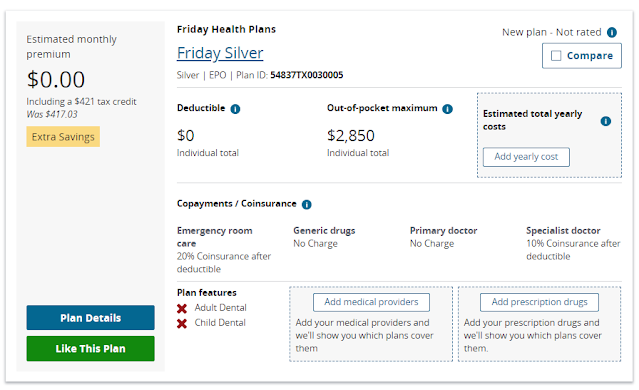
Now, suppose that first result (no subsidy) came with a rider: "subsidy eligibility for your one-person household begins at an income of $12,760." Or better yet: suppose that before I enter my income estimate, prompted by the question "What do you think your household income will be in 2021?", text below the estimate box informs me, "subsidy eligibility begins at $12,760."
Such a prompt might not make my estimate more inaccurate. When asked for income information by government, many people's learned reflex is to lowball it.
One difficulty is that this messaging would have to be provided in nonexpansion states only. Then again, the current system sends messages about Medicaid eligibility in expansion states only.
Realistically, taking advantage of the new rule abjuring low income documentation may be depend in large part on enrollment assisters and brokers. They are not -- or should not -- be in the business of encouraging clients to lie, any more than an accountant should be in the business of encouraging clients to pad expenses and deductions. But a good accountant (or tax software) will encourage a client to find and take every allowable deduction and expense. Enrollment assisters and brokers can (and do) make clients aware of the eligibility threshold, and leave no stone unturned -- flea market sales, anyone? -- in credibly estimating income that crosses the threshold.
Bigger picture: It's a legislative travesty to offer a benefit with an income threshold below which the applicant is left without help. That's not how the ACA was designed (the Supreme Court made the Medicaid expansion optional for states two years after the law's passage), and no functional legislature, federal or state, would have let such a situation fester for seven years. In the world we Americans have made ourselves, an administration that wants to govern effectively has to work around legislative dysfunction. CMS should put the threshold to the coverage gap in neon, and try to keep as many people as possible from tripping on it.
Related: In May, CMS moved quietly to shrink the coverage gap
--
* To be exact, since it takes time to retool HealthCare.gov, an applicant in this situation will first receive a request for documentation, but subsequently be informed that the information is not required. See the previous post for the explanation in the NBPP.
** Another zero-premium silver plan in this rating area has a $750 deductible -- but also a $750 annual out-of-pocket maximum, in contrast to $2,850 in the plan above (the highest allowable). In between, HealthCare.gov shows two bronze plans -- very bad deals for someone eligible for zero-premium high-CSR silver. In the wake of the subsidy boosts in the ARP, HealthCare.gov needs a lot of work.